OPERATIONAL MODEL FOR CERVICAL CANCER ELIMINATION IN KENYA
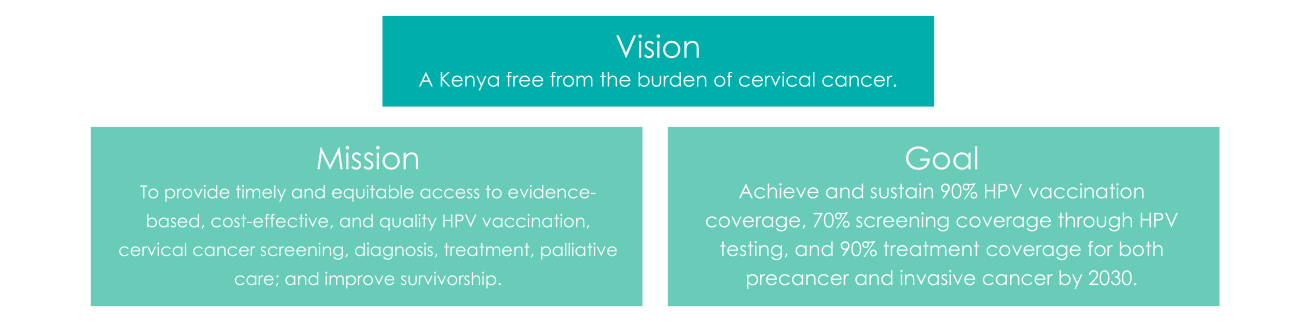
Vision, Mission, Goal
Core Values
- a. Integration
- b. Collaborations
- c. Sustainability
- d. Governance
- e. Advocacy and education
- f. Capacity building
- g. Coordination
- h. Equity
Key Result Area 1: HPV Vaccination
Operational Objectives
- Objective 1: Strengthen and expand equitable, timely, and integrated HPV vaccine delivery with the goal of achieving at least 90% coverage of girls by age 15 years, by the year 2030.
- Objective 2: Strengthen the capacity, motivation and availability of the health workforce to deliver HPV vaccines safely and effectively.
- Objective 3: Strengthen the health information system to ensure complete, timely, and integrated data capture, reporting, and decision making on HPV vaccination across public and private sectors by 2030.
- Objective 4: Strengthen the HPV vaccine supply chain for timely forecasting, equitable distribution and innovative delivery.
- Objective 5: Secure long-term domestic and external financing for HPV vaccine procurement and delivery.
- Objective 6: Promote strong political leadership, policy integration, and multi-sectoral coordination to support HPV vaccination.
- Objective 7: Promote uptake of HPV vaccination through effective behavior change messages and interventions directed at caregivers, health care providers, religious leaders, and other community influencers.
Click to View Actions
Key Result Area 2: Screening And Precancer Treatment
Operational Objectives
- Objective 1: Ensure health facilities have adequate capacity/service readiness for screening and precancer treatment.
- Objective 2: Ensure provision of quality cervical cancer screening and pre-cancer treatment services.
- Objective 3: Strengthen Health Care worker capacity for cervical cancer screening and treatment.
- Objective 4: Increase community awareness and demand creation for screening
- Objective 5: Enhance data management and use in decision making
- Objective 6: Increase financial prioritization for cervical cancer screening and treatment in national and county health budgets, as well as other financing mechanisms (costs of tests, devices, consumables, maintenance, and provider payment mechanisms)
- Objective 7: Strengthen Leadership and Governance for cervical cancer screening and precancer treatment at both national and county level
- Objective 8: Ensure quality assurance in cervical cancer screening and treatment
Click to View Actions
Key Result Area 3: Diagnosis, Treatment, Palliative And Survivorship Care For Invasive Cervical Cancer.
Operational Objectives
- Objective 1: Strengthen infrastructural capacity of comprehensive specialized facilities offering diagnostic, treatment and palliative care for cervical cancer
- Objective 2: Strengthen the availability and capacity of a well-trained, multidisciplinary oncology workforce to support timely diagnosis and comprehensive treatment of cervical cancer.
- Objective 3: Ensure availability of Health products and technologies to deliver comprehensive cervical cancer diagnosis, treatment and palliative care in counties and regional CTCs
- Objective 4: Comprehensively provide financial cover for the diagnosis and treatment of cervical cancer.
- Objective 5: Strengthen cervical cancer data systems for effective monitoring, planning, and quality improvement of diagnosis and treatment services across all levels of care.
- Objective 6: Strengthen leadership and governance systems for effective policy implementation, coordination, and oversight of cervical cancer diagnosis and treatment services at national and county levels.
Click to View Actions